Medical weight loss in Dublin, Georgia
Reach out to our bariatric navigator for more information on our program or help scheduling an appointment with a physician by calling (478) 274-3999 or you can email us. Our fax number is (478) 238-9210.
Millions of Americans struggle to maintain a healthy weight. There are a wide variety of options available today, from extreme exercise programs to trend diets that can leave you feeling discouraged and ultimately lead to weight regain. We are here to help you stop the cycle with bariatric surgical options for sustained weight loss.
At Fairview Park Hospital, our team of board-certified bariatric surgeons, nurses and registered dietitians take the time to work with you to understand what has gotten in the way of your weight loss success in the past and understand your life and long-term weight loss goals. We offer non-surgical and surgical options for weight management, and our healthcare team will work with you hand-in-hand to decide the best treatment for you, taking into account your medical history, psychological screenings and a nutrition evaluation.
Recognition
We are proud to be an Accredited Bariatric Surgery Center recognized by The American College of Surgeons Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP). This accreditation is a formal acknowledgement of our commitment to providing and supporting quality improvement and safety efforts for patients undergoing weight loss surgery. As an MBSAQIP-accredited hospital, we also hold The American College of Surgeons Surgical Quality Partner (ACS SQP) designation, which highlights our dedication to high-quality care.
We are also recognized by Blue Cross Blue Shield as a Blue Distinction Center for Bariatric Surgery.

Non-surgical weight loss options
Depending on your goals for weight loss, a non-surgical option may be the best solution. Our team provides the resources and support system you need to lose weight and keep it off. Non-surgical treatment options include:
- Customized diet programs—Through our customized diet program and nutrition counseling, we will help you develop an eating plan that fits with your lifestyle. Our certified dietitians know that too many restrictions can do more harm than good. We will work with you to evaluate your current diet, identify any nutrient deficiencies and find hidden sources of excess calories. Once we have gathered this information, we will provide a personalized nutrition plan designed to work with your personal preferences and lifestyle.
- Customized exercise programs—We provide detailed workout plans tailored to your needs, making sure your new exercise routine positively impacts your overall health. In addition to mapping out an exercise plan, we help you find ways to increase physical activity in your daily tasks and make adjustments to the role food plays in your life.
Candidates for weight loss surgery
Not everyone who wants to lose weight is a candidate for bariatric surgery. It depends on the person's body mass index (BMI) calculation, which compares your weight with your height. If you have a high BMI and an obesity-related health condition, bariatric surgery may be a good option to help you kickstart weight loss.
To better understand if you would qualify for weight loss surgery, review the following criteria:
- You are 100 pounds or more over your ideal body weight.
- You have a BMI of 40 or more.
- You have a BMI of 35 or more and are experiencing negative health effects related to obesity, such as:
- Arthritis
- Heartburn
- High blood pressure
- High cholesterol
- Obstructive sleep apnea
- Osteoarthritis
- Type 2 diabetes
- You cannot achieve a healthy body weight and sustain it for a prolonged period of time—even through medically supervised dieting.
BMI Calculator
Body Mass Index (BMI) is a number calculated from a person's weight and height. BMI provides a reliable indicator of body fatness for most people and is used to screen for weight categories that may lead to health problems.
Your BMI Score is:

All information provided by this website is intended to be general in nature and should not be used as a substitute for a visit with a health care professional. No information provided in this site may be considered medical advice. The information may not be relevant for your individual situation and may be misinterpreted. HCA assumes no responsibility for how you use information obtained from this site. Before making any decisions regarding your health care, ask your personal physician.
Surgical options for weight loss
If any of the qualifications above apply to you, talk with your doctor to see if bariatric surgery could be beneficial to your health. For those who are candidates for surgery, we provide several options. Each patient's weight loss goals differ, which is why we offer multiple surgical options to meet every person's needs. Our surgical options include adjustable gastric banding, biliopancreatic diversion with duodenal switch, gastric bypass and gastric sleeve.
Adjustable gastric banding
During adjustable gastric banding, one of our surgeons will place an inflatable band around the stomach that squeezes it to form two sections. This includes a small upper pouch and a larger lower pouch. The two sections remain connected via a small channel, which slows the rate of food as it empties from the upper pouch to the lower stomach.
After this procedure, most patients can only eat 1/2 to one cup of food before they feel full. The banding procedure facilitates weight loss by drastically reducing the amount of food you eat before feeling full. After the procedure, patients can return to their doctors' office, where the band can be adjusted.
Biliopancreatic diversion with duodenal switch
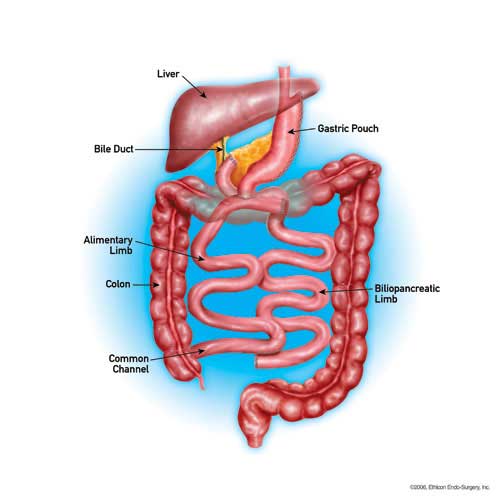
Biliopancreatic diversion with duodenal switch (BPD/DS) combines restrictive and malabsorptive weight loss techniques. The restrictive portion of the procedure involves permanently removing about 70 percent of the stomach. The malabsorptive portion reroutes a portion of the small intestine to create two separate pathways and one common channel.
The shorter of the two pathways, called the digestive loop, takes food from the stomach and brings it to the common channel. The longer pathway, known as the biliopancreatic loop, carries bile from the liver to the common channel. The common channel is part of the small intestine, about 75 to 150 centimeters in length, where the contents of the digestive path combine with the bile from the biliopancreatic loop prior to emptying into the large intestine.
The goal of creating these pathways is to reduce the amount of time the body has to absorb calories from food in the small intestine and limit the absorption of fat. Following surgery, patients only absorb about 20 percent of the fat they consume.
The primary advantage associated with BPD/DS is the combination of restrictive and malabsorptive approaches. It results in a higher percentage of excess weight loss compared to a more traditional gastric bypass procedure. Because a larger portion of the stomach is left intact compared to other procedures, patients can eat larger portions than with gastric bypass surgery.
Gastric bypass
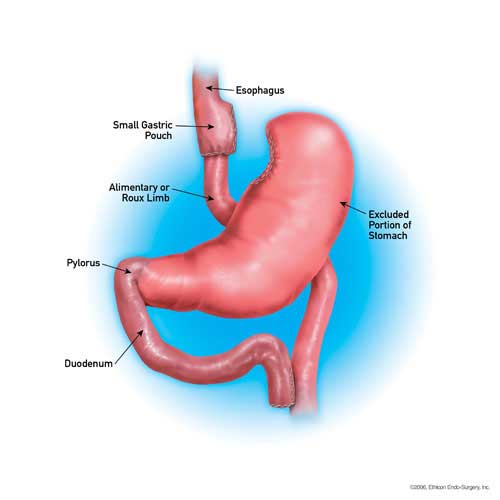
Gastric bypass, also called Roux-en-Y gastric bypass, is the most common type of weight loss surgery. Similar to the BPD/DS procedure, it applies restrictive and malabsorptive approaches to weight loss. During surgery, a surgeon divides the stomach into two parts, effectively sealing off the upper portion of the stomach from the lower portion. Next, the upper stomach is connected directly to the lower section of the small intestine.
This procedure essentially creates a shortcut for the food you consume by bypassing part of the stomach and small intestine. By skipping these parts of the digestive tract, the body absorbs fewer calories during digestion.
With this surgery, weight loss tends to be swift and dramatic. About 50 percent of total weight loss occurs within the first six months after surgery. Patients may continue to lose weight for up to two years following gastric bypass. Due to rapid weight loss, obesity-related conditions often see significant improvement.
Gastric bypass has proven, long-term results. Studies have shown that many patients keep the majority of their weight off for 10 years or longer when compared to other surgeries.
Gastric sleeve
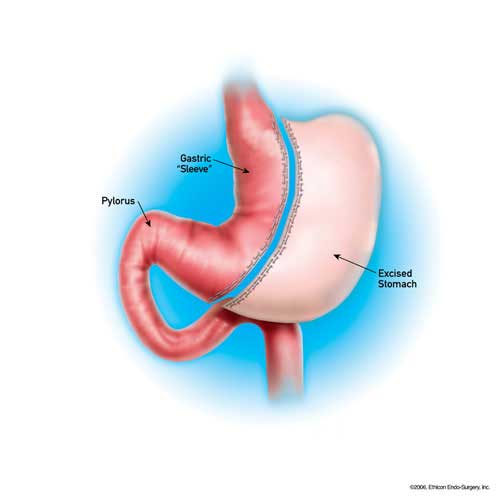
The gastric sleeve procedure, also called sleeve gastrectomy, is a restrictive procedure where 75 percent of the stomach is removed using a minimally invasive, laparoscopic approach. The remainder of the stomach forms a narrow tube, or sleeve, which connects to the intestines.
For patients who may be sick or have certain health problems, the gastric sleeve procedure offers a lower-risk way to lose weight. If needed, after a patient's weight and overall health has seen improvement—usually between 12 and 18 months—they may undergo a second procedure, such as gastric bypass. This procedure leaves the intestines unaffected, so there is no change in the way your body absorbs food and nutrients.
Free weight loss surgery seminars
We are currently offering virtual weight loss seminars. Our seminars are free and available to anyone interested in learning more about their options and required lifestyle changes when undergoing weight loss surgery. Topics we will cover include:
- Benefits and risks associated with each type of procedure
- Lifestyle changes required for weight loss success
- Steps to take before the procedure
- What to expect during the recovery process
- Who is a candidate for weight loss surgery
